
Patient Education
Discover Important Insights, the Latest News, and Information About
the World of Anesthesia
Enhancing Patient Outcomes with Specialized Anesthesia
Thank you! Your submission has been received!
Oops! Something went wrong while submitting the form.

Expert Tips That Help You Prepare for General Anesthesia
Surgery is stressful enough without feeling unprepared for what comes next. This article guides you through what to expect before and after general anesthesia, including where to find the best anesthesiologists in San Jose.
.avif)
What is Enhanced Recovery After Surgery (ERAS)?
Recovery after surgery is easier and faster with ERAS protocols. This article explains the benefits and components of ERAS as well as where to find the best anesthesiologists in San Jose who use this protocol to help patients avoid complications and recover faster.

Regional vs. Local Anesthesia: Choosing What's Right for You
If you have a procedure coming up and you’re trying to choose between local and regional anesthesia, this guide helps you understand the pros and cons of each option and where to find the best anesthesiologists in San Jose, so you’re confident in making the right choice.

Waking up After Surgery: What to Expect After Anesthesia
The thought of waking up after surgery can feel scary if you’re not sure what to expect. Get a glimpse into what post-anesthesia recovery looks like when you choose the best anesthesiologists in San Jose.
Risks & Benefits for the Top 3 Types of Anesthesia
Anesthesia makes modern surgery possible, but the type you’re given can shape how you feel during and after your procedure. This guide breaks down the differences, risks, and benefits of the top anesthesia options offered by the best anesthesiologists in San Jose.
Should I Get an Epidural for My Baby's Delivery?
The decision to get an epidural for labor pain relief is deeply personal. Learn about the best labor anesthesia practices in San Jose, including epidural facts and benefits that will help you make an informed choice that feels right for your body, your birth plan, and your baby.
4 Ways G2 Can Help You Manage Pain During Childbirth
Labor pain is one of the biggest worries expectant mothers face, but today’s medicine and supportive techniques offer more options than ever before. Explore the safe and effective ways the best anesthesiologists in San Jose make childbirth more comfortable so you can focus on welcoming your baby with confidence.
Is Anesthesia Safe for Seniors?
If you’re a senior preparing for surgery, it’s natural to have questions about anesthesia safety for the elderly. This article offers clear, compassionate guidance from the best anesthesiologists in San Jose to help you feel informed and confident every step of the way.
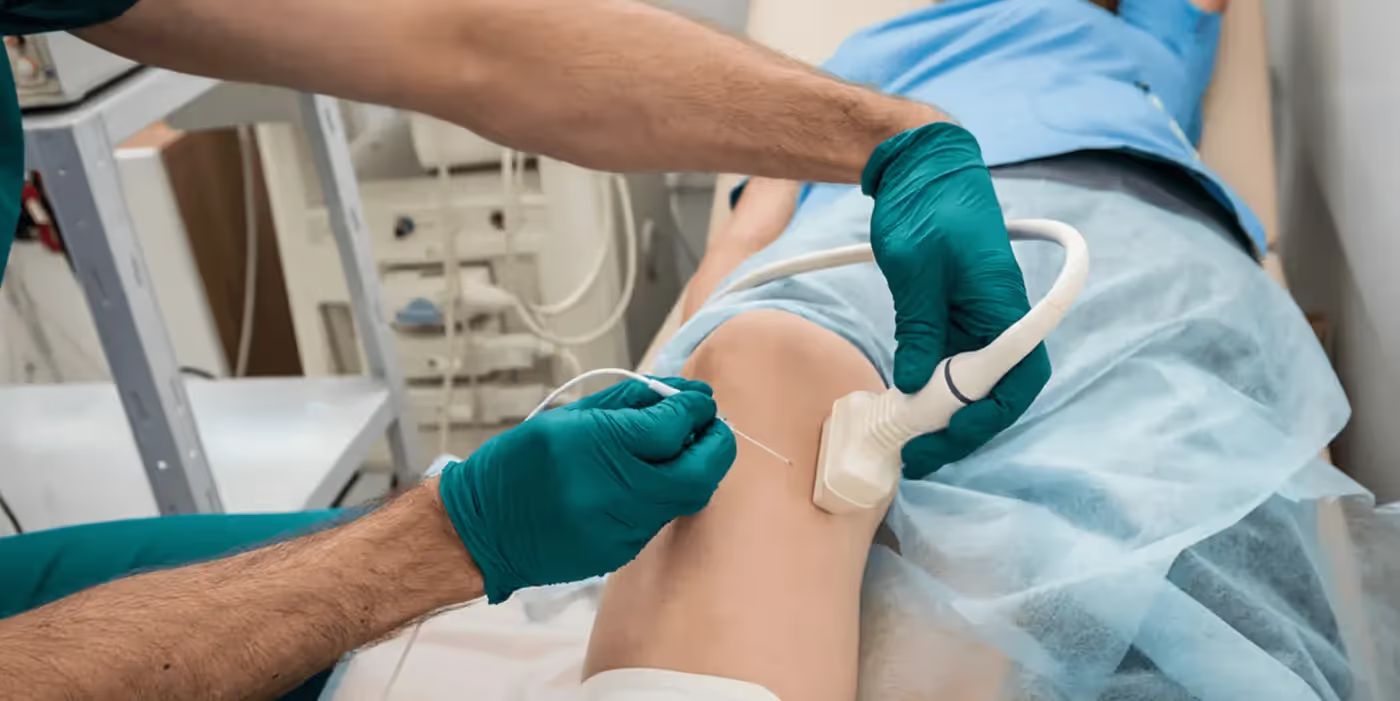
Sleep Apnea, Obesity, and Anesthesia: Know Your Risks
Surgery is never routine when conditions like obesity and undiagnosed sleep apnea are in the mix. If you're planning a procedure, understanding how these hidden risks impact anesthesia and finding the best anesthesiologists in San Jose are the most important steps you can take to protect your health.
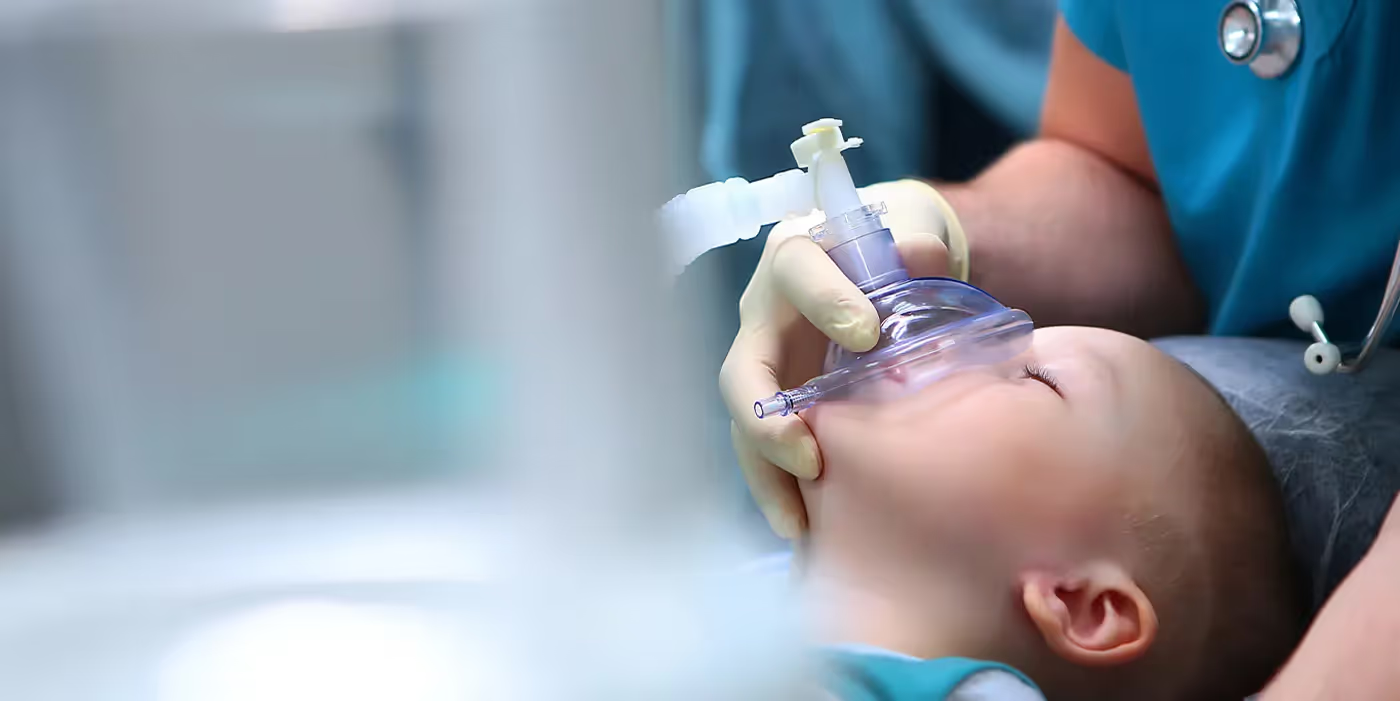
Will my Child be Safe Getting Anesthesia During Surgery?
Wondering whether anesthesia is truly safe for your child is one of the most natural concerns a parent can have before surgery. Get clarity, insight, and reassurance from the top pediatric anesthesiologists in San Jose.

Unpacking the Effects of Anesthesia on the Body
Discover what really happens when you go under, and how top anesthesiologists in San Jose ensure a safe experience.

Going Under Anesthesia Soon? Here’s What You Should Know
Anxiety about undergoing anesthesia before surgery is a common experience, but knowledge can help ease those worries. This article provides essential insights into the safety of getting anesthesia from the #1 anesthesiologist in San Jose.

The Dos and Don'ts For Preparing for Surgery
Preparing for surgery can be a nerve-wracking experience, but the right approach can make all the difference in your recovery and overall well-being. This guide will help you feel more confident and better equipped for your surgery in Los Gatos.

Do I Get to Choose My Anesthesiologist for Surgery?
Preparing for surgery and unsure about your anesthesia options? This guide covers how anesthesiologists are assigned, when you can request one, the importance of expert care, and where to find the best anesthesia providers in San Jose.

The Ultimate Guide to Anesthesia
Feeling a bit of anxiety about an upcoming surgery? This comprehensive guide will take you through everything you need to know about anesthesia, from its various types to preoperative care, pain management strategies, what to expect, and where to find the most highly skilled anesthesiologists in San Jose.








